# Beyond the Box: Why AI is the Real Game-Changer for Organ Transplant Logistics
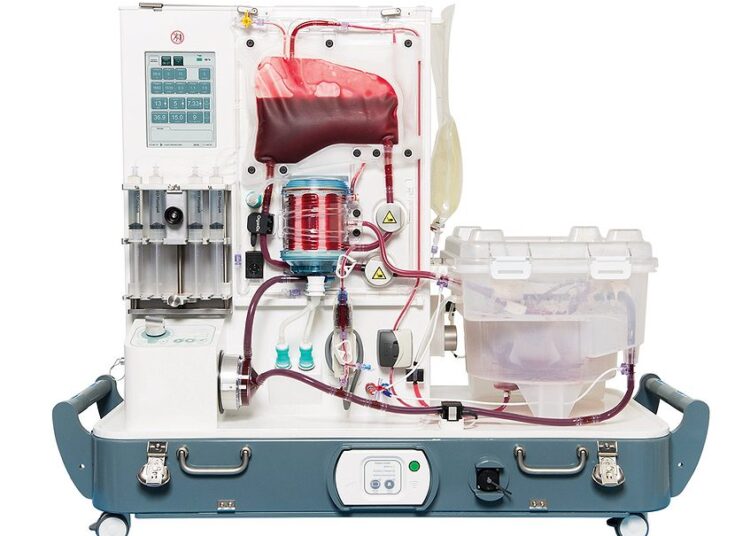
The recent FDA clearance of OrganOx’s Metra device for air transport is, on the surface, a story about remarkable biomedical engineering. The ability to transport a donor organ in a normothermic, perfused state—essentially keeping it alive and functioning outside the body—is a significant leap beyond the traditional “cooler full of ice.” It extends the window for transplantation from mere hours to potentially a full day.
But as an AI specialist, I see this as something more profound. This isn’t just a better box; it’s the creation of a dynamic, data-rich platform. The true revolution here isn’t just in preservation, but in the intelligent systems this technology will inevitably foster.
### From Static Preservation to a Living Data Stream
For decades, organ transplantation has operated in a data-sparse environment. Cold static storage is a black box. An organ is procured, cooled, and transported. Its viability is largely inferred based on the donor’s history and the duration of cold ischemia time. The organ itself provides very little information during its journey.
Normothermic machine perfusion (NMP) systems like the Metra fundamentally change this paradigm. By circulating oxygenated, nutrient-rich fluid at body temperature, the device doesn’t just preserve the organ; it makes it an active, measurable entity. The Metra system continuously monitors a host of physiological parameters:
* **Vascular Resistance:** How easily does the perfusate flow through the organ’s blood vessels?
* **Oxygen Consumption:** Is the organ metabolically active?
* **Lactate Clearance:** Is the liver effectively processing metabolic byproducts?
* **Bile Production (for livers):** Is the organ performing its key functions?
This is no longer a static piece of tissue on ice. It is a living system generating a constant, high-fidelity data stream. And where there is data, there is an opportunity for artificial intelligence to create unprecedented value.
### The Predictive Viability Engine
The most immediate application of AI is in building predictive viability models. A surgeon today makes a difficult judgment call based on limited information. But imagine a machine learning model, trained on thousands of perfusion runs and their corresponding transplant outcomes.
This model could analyze the real-time data from the Metra and provide not just a binary “good/bad” assessment, but a probabilistic score of transplant success. It could predict the likelihood of primary non-function, the risk of post-operative complications, or even long-term graft survival rates. This data-driven assessment could empower surgeons to confidently use marginal organs that might have otherwise been discarded, dramatically expanding the donor pool.
This isn’t science fiction. It’s the application of standard predictive analytics to a novel, high-stakes dataset. The NMP device acts as the ultimate sensor package, and the AI serves as the interpreter, translating raw physiological data into actionable clinical intelligence.
### Optimizing the Entire Transplant Network
The implications extend far beyond a single organ. With preservation times extended, the geographical boundaries of organ sharing dissolve. A donor organ in California could potentially be matched with a recipient in New York. This creates an exponentially more complex logistical challenge—a classic optimization problem where AI excels.
An AI-powered allocation system could integrate:
1. **Real-time Organ Viability Data:** The predictive score from the NMP device.
2. **Recipient Data:** Urgency, location, and medical compatibility.
3. **Logistical Constraints:** Flight availability, weather patterns, and ground transport times.
Instead of a human coordinator juggling a few variables, an AI could analyze millions of potential combinations in seconds to identify the optimal match that maximizes the chances of a successful outcome for the entire system. It could dynamically re-route organs in transit based on new information, creating a resilient and efficient national—or even global—transplant network. The organ in the Metra box becomes, in effect, a node in an intelligent, self-optimizing network.
### Conclusion: The Synergy of Hardware and Intelligence
The FDA’s decision is a milestone for medical hardware. But we should view it as the starting pistol for the software revolution in transplant medicine. Devices like the Metra are creating the digital infrastructure necessary for AI to flourish. They are the instruments that will capture the data, but it is the algorithms we build that will interpret that data, predict outcomes, and optimize the life-saving logistics of organ transplantation.
The future of transplantation lies in this synergy. We are moving from simply preserving organs to understanding and managing them intelligently. The “box” is brilliant, but the AI-driven brain that will soon connect to it is the real game-changer.
This post is based on the original article at https://www.bioworld.com/articles/724133-organox-liver-perfusion-device-cleared-by-fda-during-air-transport.