### Beyond the Hype: Why Real-World Data Still Favors Bariatric Surgery Over GLP-1s
The current discourse around weight management is dominated by the meteoric rise of GLP-1 receptor agonists. Drugs like semaglutide and tirzepatide have captured the public imagination and shaken the healthcare industry, positioned as revolutionary tools in the fight against obesity. From a data perspective, the initial clinical trial results were impressive. But as AI and data science professionals know, the true test of any intervention isn’t in the pristine, controlled environment of a trial—it’s in the messy, complex, and unpredictable real world.
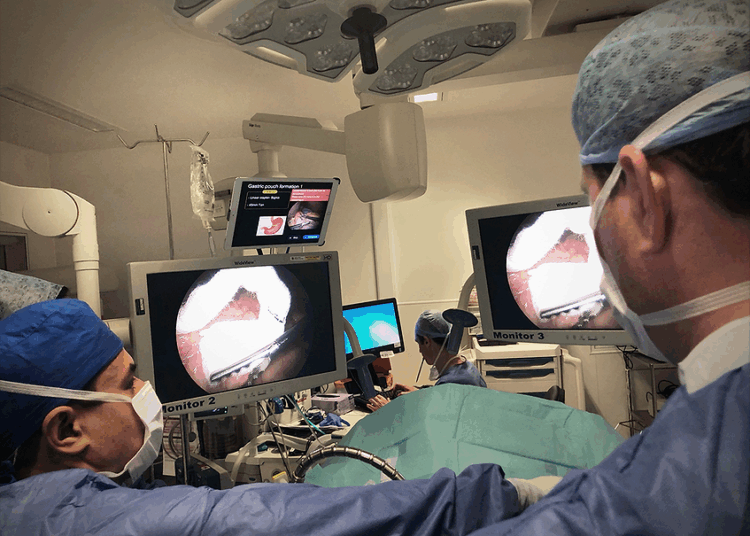
A recent retrospective study published in *JAMA Surgery* provides a crucial dose of that real-world evidence, and the signal it sends is clear: bariatric surgery remains the gold standard for significant, sustained weight loss. For medical device manufacturers in this space, this data is not just comforting; it’s a powerful validation of the enduring value of surgical intervention.
—
#### The Signal in the Noise: A Real-World Data Showdown
The study compared one-year outcomes for patients who underwent bariatric surgery (specifically sleeve gastrectomy or gastric bypass) against a matched cohort prescribed GLP-1 or GLP-1/GIP receptor agonists. The results were not just different; they were orders of magnitude apart.
* **Bariatric Surgery Patients:** Achieved an average total body weight loss of **27.9%**.
* **GLP-1/GIP Medication Patients:** Achieved an average total body weight loss of **10.5%**.
The conclusion is numerically stark: on average, surgery produced nearly three times the weight loss of medication alone.
From a machine learning perspective, this is a classic example of why real-world evidence (RWE) is an invaluable, and fundamentally different, data source compared to Randomized Controlled Trials (RCTs). RCTs are designed to isolate a single variable—the drug’s efficacy—in a highly compliant, carefully selected population. RWE, on the other hand, captures the confounding variables that define reality: imperfect adherence, comorbidities, socioeconomic factors, and patient motivation.
The discrepancy in these results likely points to a key variable that is notoriously difficult to model: long-term human behavior. A surgical procedure is a singular, definitive event that fundamentally alters the body’s physiological and hormonal systems related to satiety and metabolism. Its efficacy is not dependent on a patient remembering to take a weekly injection, managing side effects, or navigating insurance hurdles for refills month after month. The “adherence” to the primary intervention is, in effect, 100%. GLP-1s, for all their power, are dependent on a long chain of consistent patient action, a factor where real-world performance almost always diverges from clinical trial ideals.
#### The Future is Not a Binary Choice, It’s a Personalized Pathway
This data should not be interpreted as a simple “win” for surgery over pharmaceuticals. Instead, it should be seen as a critical input for a more sophisticated, AI-driven model of obesity care. The ultimate question is not “Which treatment is better?” but rather, **”Which treatment is optimal for *this specific patient*?”**
This is where predictive analytics and machine learning will redefine the field. We are moving beyond one-size-fits-all protocols and toward deeply personalized treatment pathways. Imagine an AI model that synthesizes a patient’s entire data profile:
* **Genomic markers** for metabolic response
* **Electronic Health Record (EHR) data** on comorbidities and treatment history
* **Behavioral data** indicating likely adherence to a medication regimen
* **Risk models** for surgical complications
This system wouldn’t just present a doctor with options; it would provide a probabilistic forecast of outcomes for each potential pathway. It might identify one patient as an ideal candidate for surgery, predicting high success and low risk. For another, it might flag a high risk of non-adherence to medication, suggesting a more definitive intervention is necessary. Conversely, it could identify a patient for whom the risks of surgery outweigh the benefits and for whom a GLP-1, perhaps combined with digital coaching, is the optimal starting point.
Furthermore, AI can help orchestrate hybrid approaches. A model might suggest an initial course of GLP-1s to reduce a patient’s weight and comorbidities, thereby lowering their surgical risk profile and making them a better candidate for a subsequent bariatric procedure.
—
#### Conclusion: Data Reaffirms a Cornerstone of Care
The *JAMA Surgery* study serves as a vital anchor in a sea of hype. It uses real-world data to reaffirm that bariatric surgery is an incredibly potent intervention, delivering transformative results that, at present, pharmacotherapy alone cannot match. For the MedTech industry, this is a clear signal that the devices and tools enabling these procedures are not being replaced, but rather are being positioned as a powerful component within an increasingly sophisticated, data-driven ecosystem of care.
The rise of GLP-1s doesn’t diminish the role of surgery; it clarifies it. The future of obesity treatment will not be a battle between pills and procedures, but a synergy orchestrated by intelligent systems that leverage the strengths of every available tool to chart the best course for every individual patient.
This post is based on the original article at https://www.bioworld.com/articles/724213-surgery-results-in-3-times-more-weight-loss-than-glp-1s.